Understanding Plantar Fasciitis: Causes, Symptoms, and Treatment
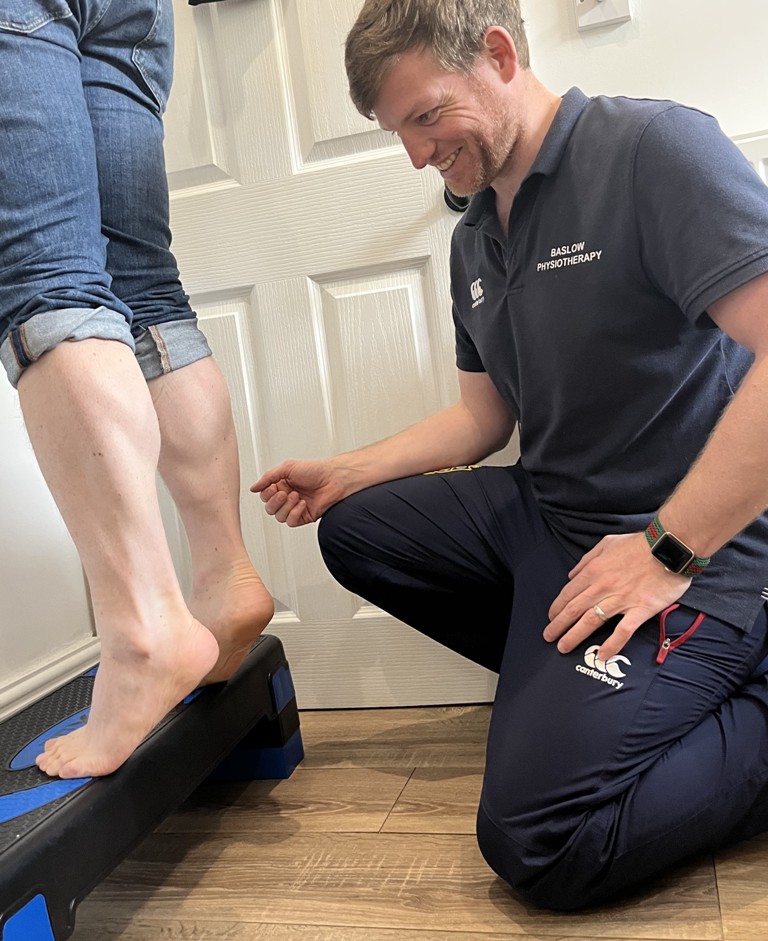
Plantar fasciitis is one of the most common causes of foot pain worldwide. The thick band of tissue running from the big toe to your heel on the inside arch of your foot becomes inflamed. There are a number of risk factors that can contribute to potentially having this problem, including age, sex, weight, footwear and training. Understanding the causes, symptoms and treatment options help you to manage this problem effectively.
What is Plantar Fasciitis?
The plantar fascia is a fibrous band of tissue that connects the heel bone to the toes, providing support to the arch of the foot. When this tissue becomes overused or strained, it can lead to micro-tears, causing inflammation and pain. Plantar fasciitis most commonly affects the heel, but pain can also be felt along the bottom of the foot.

foot pain with walking
Causes of Plantar Fasciitis
Several factors can contribute to the development of plantar fasciitis, including:
- Overuse or Repetitive Stress: Activities like running, dancing, or standing for long periods can put repetitive stress on the plantar fascia, leading to inflammation.
- Foot Structure: People with high arches, flat feet, or abnormal walking patterns (such as excessive pronation) are at greater risk of developing plantar fasciitis. These conditions place added stress on the fascia.
- Obesity: Carrying extra weight puts more strain on your feet, increasing the likelihood of developing plantar fasciitis.
- Improper Footwear: Shoes that lack proper arch support or cushioning, such as flip-flops or worn-out sneakers, can contribute to the development of this condition.
- Age: Plantar fasciitis is most common in people between the ages of 40 and 60, thought to be due to hormonal changes as we age.
- Tight Muscles: Tight calf muscles or Achilles tendons can increase tension on the calcaneus (heel bone) stressing the plantar fascia, leading to inflammation.
Symptoms of Plantar Fasciitis
The hallmark symptom of plantar fasciitis is pain in the heel, particularly during the first steps out of bed in the morning or after periods of inactivity. The pain typically decreases as you start walking but may return after long periods of standing or excessive activity.
Other common symptoms include:
- Pain in the bottom of the heel: The pain is often sharp or stabbing, especially when you stand up after sitting or lying down.
- Tenderness: The affected area of the foot may be tender to the touch, especially near the heel.
- Swelling: Mild swelling may occur in the heel or arch of the foot.
Diagnosing Plantar Fasciitis
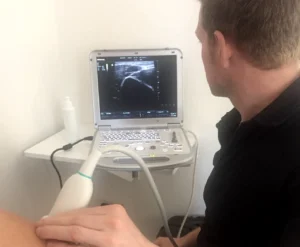
Guy the musculoskeletal clinical specialist would complete a thorough assessment including questions to identify risk factors that may have contributed to the symptoms. This would be followed by a physical examination of strength, flexibility and possibly involving diagnostic real time ultrasound imaging of the structures involved under the foot to rule out other potential causes of heel pain, like fractures or bone spurs.
Treatment Options for Plantar Fasciitis
The goal of treatment is to reduce inflammation, relieve pain, and prevent future injury. Common treatment options include:
- Rest and Activity Modification: Taking a break from activities that aggravate the condition, such as running or standing for long periods, is crucial for allowing the plantar fascia to heal. Switching to low-impact exercises, like swimming or cycling, may help maintain fitness without exacerbating the pain.
- Stretching Exercises: Stretching the calves, Achilles tendons, and the plantar fascia itself can help relieve tension and reduce pain. A common exercise is the “towel stretch,” where you use a towel to stretch the bottom of your foot before getting out of bed or rolling a ball under your foot.
- Ice Therapy: Applying ice to the affected area can help reduce inflammation and alleviate pain. Try rolling a frozen water bottle under the foot or applying an ice pack directly to the heel for 15-20 minutes at a time.
- Footwear Modifications: Wearing shoes with good arch support and cushioning is essential in relieving the pressure on the plantar fascia. Avoid walking barefoot on hard surfaces, and consider using orthotic insoles to provide additional support.
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Over-the-counter NSAIDs like ibuprofen or naproxen can help reduce pain and inflammation. However, these should only be used for short-term relief.
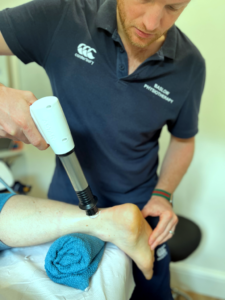
- Physiotherapy: Appropriate exercises to stretch and strengthen the leg and foot will be provided tailored to your specific needs. Alongside therapeutic techniques like ultrasound therapy, shockwave therapy and deep tissue massage to reduce inflammation and improve flexibility.
- Corticosteroid Injections: In cases where pain persists despite conservative treatment, corticosteroid injections may be used to reduce inflammation and provide more significant pain relief. However, these injections are typically reserved for severe cases.
- Night Splints: Wearing a night splint can help keep the foot in a dorsiflexed position while you sleep, gently stretching the plantar fascia and Achilles tendon. This can help prevent morning pain and stiffness.
 =
=
Prevention Tips
While plantar fasciitis can be challenging to recover from, there are several steps you can take to prevent it from occurring or recurring:
- Wear proper footwear: Choose shoes with good arch support and cushioning to minimize stress on the feet.
- Avoid high-impact activities: Opt for low-impact exercises that are easier on your feet.
- Maintain a healthy weight: Reducing excess weight can reduce the strain on your feet and lower your risk of developing plantar fasciitis.
- Stretch regularly: Incorporate stretching exercises for your calves, hamstrings, and feet into your daily routine to maintain flexibility.
- Gradually increase activity: Avoid sudden increases in the intensity or duration of physical activity to prevent overuse injuries.
- Strengthening foot muscles: By strengthening the muscles that support your foot will take pressure off the plantarfascia.
Final Thoughts
Plantar fasciitis can be a painful and frustrating condition, but with the right approach to treatment and prevention, most people can recover and resume their normal activities. If you experience persistent heel pain, please come for an assessment at Baslow Physiotherapy for an accurate diagnosis and personalised treatment plan. Drop Guy an email.
By understanding the causes, symptoms, and available treatment options for plantar fasciitis, you can take the necessary steps to alleviate pain and prevent future episodes, ultimately improving your quality of life and foot health.